Mon - Fri: 8 am - 5 pm
(407) 888-5980
(407) 888-2492

Best Endocarditis Treatment in Orlando
Advanced Care & Endocarditis Treatment in Orlando
Infective endocarditis is a rare but life-threatening infection of the heart’s inner lining or its valves. This condition remains a significant clinical challenge because it involves a complex battle between aggressive pathogens and the body’s most vital organ.
Typically caused by bacteria or fungi entering the bloodstream, the infection settles on damaged or artificial heart tissue, forming clumps of germs known as vegetations. If left untreated, these vegetations can destroy heart valves, lead to heart failure, or break off and travel to other parts of the body, potentially causing strokes or organ damage.
Because the symptoms—such as persistent fever, fatigue, and body aches—can often mimic those of the common flu, early diagnosis is critical. In Orlando, patients have access to advanced diagnostic tools and specialized oversight of infectious diseases to ensure that treatment is both rapid and effective.
In this guide, we will explore the different types of endocarditis, the underlying causes, and the advanced treatment protocols used to achieve a successful cure. Whether you are a patient, a caregiver, or simply looking to understand heart health, this overview provides the essential facts you need to know.
How Endocarditis Disease Affects Your Heart: Three Stages of Endocarditis
Endocarditis is a life-threatening inflammation that targets the endocardium, the smooth, innermost layer of the heart's chambers and valves. To understand it fully, it is helpful to look at it as a three-stage process:
1. Entry into the Bloodstream
The heart is normally well-protected, but certain activities can introduce pathogens into the blood (a condition called bacteremia). This can happen through something as simple as a dental cleaning that causes bleeding gums, or through more direct routes like intravenous drug use, surgery, or indwelling medical catheters.
2. Attachment to the Heart
Healthy heart tissue is slippery and resistant to bacteria. However, if a person has a pre-existing heart condition—such as a scarred valve from rheumatic fever, a prosthetic valve, or a congenital heart defect—the surface is often rougher. This allows circulating bacteria or fungi to "snag" and attach themselves to the tissue.
3. Formation of Vegetations
Once attached, the pathogens multiply and become encased in a "protective" layer of platelets and fibrin (clotting proteins). This clump is known as vegetation. These growths are dangerous for two main reasons:
-
Mechanical Damage: They can prevent heart valves from closing properly, leading to heart failure as blood leaks backward (regurgitation).
-
Embolization: Because these clots are fragile, pieces can break off and travel through the arteries. If a piece lodges in the brain, it causes a stroke; if it enters the lungs, it causes a pulmonary embolism.

Types of Endocarditis
1. Acute Infective Endocarditis
This is a medical emergency. It involves a sudden, violent onset of symptoms and can destroy heart valves in just a few days.
-
The Pathogen: Most commonly caused by Staphylococcus aureus (often referred to as "Staph"). This bacterium is highly aggressive and can attack even a perfectly healthy heart valve.
-
The Symptoms: High fever, rapid heart rate, and extreme fatigue.
-
The Risk: Because it progresses so quickly, acute endocarditis often leads to heart failure or severe embolisms (clumps of bacteria breaking off) shortly after the infection begins.
2. Subacute Infective Endocarditis
This version is more "stealthy." It develops slowly over several weeks or even months, making it much harder to diagnose early.
-
The Pathogen: Usually caused by less aggressive bacteria like Viridans streptococci (often found in the mouth).
-
The Symptoms: Vague, flu-like symptoms such as low-grade fever, night sweats, weight loss, and general body aches.
-
The Risk: Because it feels like a lingering cold, patients may delay seeking care, allowing the bacteria to slowly erode the heart valves over time.
3. Prosthetic Valve Endocarditis (PVE)
This occurs specifically in patients who have had a heart valve replaced with a mechanical or biological (animal tissue) valve.
Biofilm Challenges: Bacteria can attach to the artificial surface of a prosthetic valve and create a "biofilm"—a slimy, protective shield that makes it nearly impossible for antibiotics to penetrate.
Timing Matters:
-
Early PVE: Occurs within a year of surgery, often due to contamination during the procedure.
-
Late PVE: Occurs more than a year later, usually from bacteria entering the blood through dental work or other infections.
-
The Risk: This type of endocarditis has a higher mortality rate and frequently requires a second surgery to replace the infected artificial valve.
4. Culture-Negative Endocarditis
In about 5% to 10% of cases, standard blood tests do not grow any bacteria, even though the patient shows clear signs of heart infection on an echocardiogram.
Why it Happens: * The patient may have already started antibiotics before the blood was drawn.
-
The infection is caused by "fastidious" organisms—rare germs that are very difficult to grow in a lab.
-
The cause is non-bacterial, such as a fungus.
The Solution: Specialized labs at clinics like Sunshine Specialty Healthcare must use advanced molecular testing (like PCR) to identify the "hidden" germ and choose the correct medication.
Causes and Risk Factors: How Germs Reach the Heart
The heart is normally a sterile environment. Endocarditis begins when the blood becomes contaminated with bacteria or fungi, a state known as bacteremia.
-
Dental Issues: The mouth is home to millions of bacteria. Activities that cause bleeding—such as professional dental cleanings, extractions, or even severe gum disease (periodontitis)—provide a direct "highway" for bacteria like Streptococcus to enter the bloodstream.
-
Skin Entry: The skin is the body's primary barrier. Puncturing this barrier through tattoos, body piercings, or the use of unsterile needles in intravenous (IV) drug use allows aggressive germs like Staphylococcus aureus to bypass the immune system.
-
Medical Devices: Modern life-saving devices can inadvertently act as bridges for infection. Long-term IV catheters, pacemakers, and prosthetic heart valves provide "non-living" surfaces where bacteria can attach and grow without interference from the body's natural defenses.
-
Underlying Heart Conditions: Pathogens are much more likely to settle on heart tissue that is already scarred or abnormal. This includes people with congenital heart defects, valves damaged by rheumatic fever, or age-related calcium buildup.
Recognizing the Warning Signs: Endocarditis Symptoms
Because endocarditis can progress either rapidly (acute) or slowly over several months (subacute), the symptoms can vary greatly from person to person. Many early Endocarditis symptoms are "non-specific," meaning they often mimic a stubborn flu or a general infection.
Recognizing these "red flags" early is the key to preventing permanent heart valve damage. Common Endocarditis symptoms are :
1. Common "Flu-Like" Symptoms
In many cases, the first signs of endocarditis are systemic, affecting the whole body as it tries to fight the infection:
-
Persistent Fever and Chills: A fever that doesn't go away or keeps returning is the most common symptom.
-
Night Sweats: Waking up with soaked sheets or clothing, even if the room is cool.
-
Fatigue: An overwhelming sense of tiredness or weakness that doesn't improve with rest.
-
Aching Joints and Muscles: General body aches similar to those felt during a viral infection.
2. Heart-Related Warning Signs
As the infection settles on the heart valves, it can change how blood flows through the heart:
-
New or Changed Heart Murmur: This is often the most significant clinical sign. A doctor may hear a "whooshing" sound caused by blood leaking past an infected valve.
-
Shortness of Breath: Difficulty breathing, especially during physical activity or when lying flat, which can indicate the beginning of heart failure.
-
Chest Pain: Discomfort or pressure when breathing.
3. Visible Physical Indicators (Skin & Eyes)
Endocarditis Disease can cause unique, visible markers due to broken blood vessels or immune system reactions:
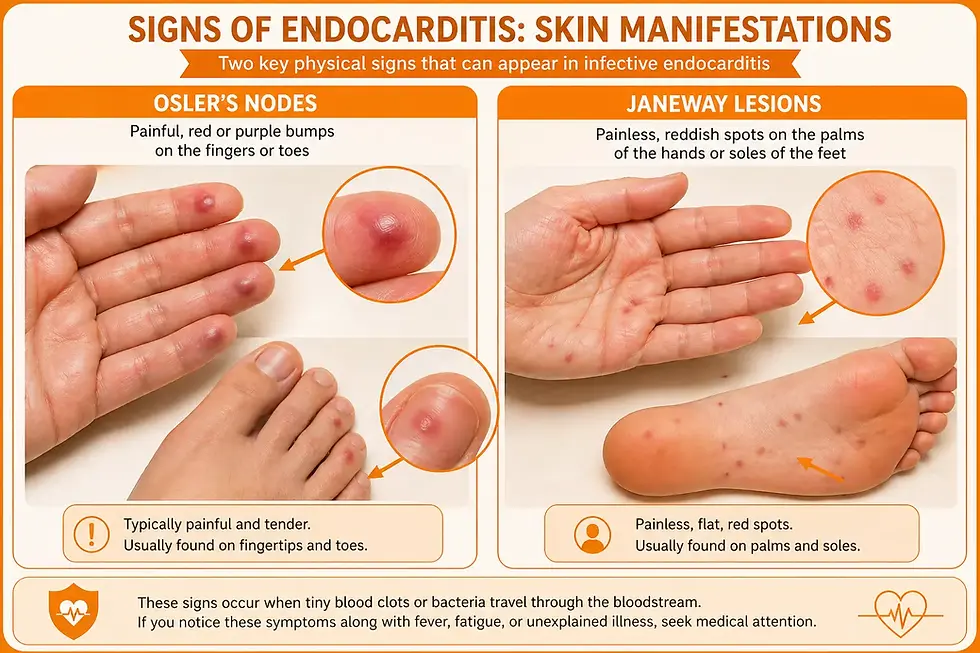
-
Janeway Lesions: Small, painless red spots on the palms of the hands or soles of the feet.
-
Osler’s Nodes: Small, painful, red-to-purple bumps on the tips of the fingers or toes.
-
Petechiae: Tiny purple or red spots on the skin, the whites of the eyes, or inside the mouth, caused by broken capillaries.
-
Splinter Hemorrhages: Thin, dark reddish-brown lines under the fingernails or toenails that look like tiny wood splinters.
4. Symptoms of Embolism (Advanced Signs)
If a "vegetation" (clump of bacteria) breaks off and travels through the bloodstream, it can cause sudden, severe symptoms depending on where it lands:
-
Sudden Confusion or Weakness: Signs of a stroke if a fragment reaches the brain.
-
Pain in the Side or Abdomen: Often caused by a fragment lodging in the spleen or kidneys.
-
Cold, Pale, or Painful Extremity: Occurs if a fragment blocks blood flow to an arm or leg.

Identifying the Infection: Endocarditis Diagnosis
Because endocarditis can mimic other illnesses, doctors use a multi-step "detective" process to confirm the diagnosis. In clinical settings, this is often guided by the Modified Duke Criteria, a standardized set of requirements that combine laboratory results with physical findings.
1. Blood Cultures: Identifying the Pathogen
The most critical step in an endocarditis diagnosis is the blood culture.
-
The Process: A clinician will draw multiple sets of blood from different veins over 24 hours.
-
The Goal: To identify the exact bacteria or fungi causing the infection.
-
The Clinical Benefit: Knowing the specific "germ" allows your specialist to move from broad-spectrum drugs to a targeted antibiotic, ensuring maximum effectiveness with fewer side effects.
2. Echocardiogram: Visualizing the Heart
An echocardiogram uses sound waves to create a live image of your heart. Doctors look for "vegetations"—the telltale clumps of bacteria and blood cells.
-
Transthoracic Echocardiogram (TTE): A standard ultrasound where the probe is moved over your chest. It is non-invasive and usually the first test performed.
-
Transesophageal Echocardiogram (TEE): If the TTE isn't clear enough, a TEE is used. A small probe is passed down the esophagus (the tube connecting your throat to your stomach). Because the esophagus sits right behind the heart, this provides a much more detailed, high-resolution view of the valves.
3. Blood Tests for Inflammation
While not specific to the heart, certain blood markers help confirm that the body is fighting a significant infection:
-
CBC (Complete Blood Count): Often shows a high white blood cell count, indicating an active immune response.
-
CRP (C-Reactive Protein) & ESR (Sedimentation Rate): These tests measure levels of general inflammation in the body. If these levels stay high, the infection is likely still active.
4. Advanced Imaging and Tests
In complex cases, especially those involving prosthetic valves or pacemakers, additional tests may be required:
-
Electrocardiogram (ECG/EKG): Used to check if the infection is interfering with the heart’s electrical signals, which can cause an irregular heartbeat (arrhythmia).
-
Chest X-ray: To see if the infection has caused the heart to enlarge or if fluid has built up in the lungs (a sign of heart failure).
-
CT or MRI Scans: If doctors suspect the infection has spread or that a piece of vegetation has broken off (embolism), they may scan the brain, spleen, or other organs.
Importance Of Early Detection
Because endocarditis can mimic a lingering flu with symptoms like fever, chills, and fatigue, it is often missed in its early stages. Without specialized treatment, the infection can permanently destroy heart valves, leading to the need for open-heart surgery. Expert infectious disease oversight is required to ensure the correct antimicrobial is used to penetrate these dense, protective vegetations.
When to See a Specialist
If you have a known heart condition, a prosthetic valve, or a history of heart defects, you should contact Dr. Jose A. Giron immediately if you develop a persistent fever or unexplained fatigue.
Clinical Note: Do not wait for "classic" signs like Janeway lesions to appear. Most patients will only experience fever and fatigue in the early stages. Early blood cultures are the only way to confirm the diagnosis.
Cure & Endocarditis Treatment in Orlando, Sunshine Specialty Healthcare
Curing endocarditis is a marathon, not a sprint. Because the infection is buried inside dense "vegetations" on the heart valves, treatment must be sustained and powerful.
-
Targeted IV Antibiotics: Treatment almost always requires intravenous (IV) therapy because oral pills cannot achieve high enough concentrations in the blood to penetrate heart vegetations.
-
Vancomycin is often used for resistant strains.
-
Ceftriaxone or Penicillin G is used for highly sensitive bacteria.
-
The standard duration is 4 to 8 weeks to ensure every single germ is killed.
-
Surgical Intervention: About 50% of cases require surgery. This is not a failure of the antibiotics, but a necessity if the infection has physically destroyed a valve, caused a heart abscess, or if the "clump" of bacteria is so large that it is likely to break off and cause a stroke.
-
Expert Oversight: This is a high-stakes infection. Management by an infectious disease specialist like Dr. Jose A. Giron is vital to balance the high doses of medication needed with the safety of your kidneys and liver.
-
Successful treatment for endocarditis involves two primary goals: eliminating the underlying infection and repairing any structural damage to the heart valves. At specialized centers like Sunshine Specialty Healthcare and the Orlando Health Heart & Vascular Institute, treatment is improved to the specific pathogen involved.
Prevention Strategies: Protecting Your Heart
For those at high risk, prevention is the most effective way to avoid life-threatening complications.
-
Antibiotic Prophylaxis: According to 2026 clinical standards, patients with artificial valves or certain congenital heart defects should take a specific dose of antibiotics shortly before dental work or certain surgeries to kill any bacteria that might enter the blood during the procedure.
-
Excellent Oral Hygiene: Maintaining healthy gums and teeth is the simplest way to reduce the daily "leaking" of bacteria into your blood. Regular brushing, flossing, and professional cleanings are essential preventative measures.
-
Skin Integrity: Protect your skin and avoid unnecessary risks. If you are in a high-risk category for heart issues, it is generally advised to avoid new piercings or tattoos. If you do sustain a skin injury, clean it immediately and monitor for signs of infection like redness or swelling.
Recovery Timeline: How Long Does Endocarditis Treatment in Orlando Take?
Because the bacteria in endocarditis are buried deep within the heart's "vegetations" (clumps of germs and blood cells), they are difficult for the immune system and antibiotics to reach. As a result, treatment requires a significantly longer duration than a standard infection to ensure a total cure.
1. Standard Endocarditis Treatment Duration (4 to 8 Weeks)
For most patients, long-term intravenous (IV) antibiotics are mandatory. The exact length of your course depends on three factors: the type of bacteria, whether you have a natural or artificial valve, and how quickly your body responds to the medication.
-
Native Valve Endocarditis (4 to 6 Weeks): If the infection is on your original heart valve, a 4-to-6-week course is the standard protocol to prevent a relapse.
-
Prosthetic Valve Endocarditis (6 to 8+ Weeks): Bacteria attach more stubbornly to artificial materials (biofilm). Treating an infected prosthetic valve often requires a minimum of 6 weeks, sometimes extending to 8 weeks or longer.
-
Fungal Endocarditis: These are the most difficult cases to treat and often require several months of medication, frequently followed by lifelong suppressive therapy.
2. The "Switch" to Home-Based Care (OPAT)
You do not always have to stay in the hospital for the entire duration. Under the guidelines followed by Dr. Jose A. Giron, stable patients may transition to OPAT (Outpatient Parenteral Antimicrobial Therapy).
-
Weeks 1–2: Usually spent in the hospital for stabilization and to ensure no immediate heart failure or stroke risks exist.
-
Weeks 3–8: Once stable, you may receive your IV doses at home with the help of a visiting nurse or at an outpatient infusion center.
3. Surgical Recovery Timeline
If the infection has damaged your heart valves, surgery may be performed during the initial antibiotic phase.
Post-Surgery Antibiotics: Even if the infected valve is removed, the 2026 clinical guidelines mandate that the antibiotic clock often "restarts" or continues for at least 6 weeks post-surgery to ensure the new valve does not become reinfected.
Treatment Timelines at Sunshine Specialty Healthcare, Orlando
Critical Note: Never miss a dose or stop your IV therapy early. Even if you feel 100% healthy by week three, the bacteria deep inside the heart vegetations can survive and cause a life-threatening "rebound" infection if the full course isn't completed.
Endocarditis Treatment Clinical Guidelines at Sunshine Specialty Healthcare
At our Orlando facility, Dr. Jose A. Giron follows the most recent AHA (American Heart Association) and IDSA (Infectious Diseases Society of America) guidelines to ensure patient safety:
-
Pathogen-Specific Therapy: We prioritize identifying the exact germ via blood cultures before finalizing a long-term medication plan.
-
OPAT (Outpatient Parenteral Antimicrobial Therapy): We facilitate home-based IV treatment for stable patients, allowing for a more comfortable recovery outside the hospital.
-
Weekly Clinical Monitoring: Guidelines mandate weekly blood work to monitor kidney and liver function while on high-potency antibiotics.
-
Echocardiographic Surveillance: We use advanced imaging to monitor the heart's healing progress and detect any potential complications early.
Common Medications for Endocarditis
Because the bacteria in endocarditis are often trapped within dense "vegetations" on heart valves, treatment requires high-potency medications for Endocarditis delivered directly into the bloodstream. At Sunshine Specialty Healthcare, the choice of medication is never "one size fits all"—it is precisely tailored to the specific pathogen identified in your blood cultures.
1. The "Heavy Hitters": Common Antibiotics
The majority of cases are caused by Gram-positive bacteria like Staphylococcus or Streptococcus. To combat these, doctors typically use:
-
Vancomycin: Often the first line of defense, especially if a resistant strain like MRSA is suspected. It is a powerful antibiotic that requires careful monitoring of blood levels to ensure it is effective without harming the kidneys.
-
Ceftriaxone: A common choice for streptococcal infections. It is often preferred for home-based IV therapy (OPAT) because it can typically be administered just once a day.
-
Penicillin G: Despite being one of the oldest antibiotics, it remains the "gold standard" for treating many highly sensitive strains of Streptococcus found in the mouth.
-
Nafcillin or Oxacillin: These are the preferred medications for Endocarditis if the bacteria is confirmed to be a standard, non-resistant strain of Staphylococcus aureus.
-
Gentamicin: Often used as a "synergist." While it isn't usually used alone, adding a low dose of Gentamicin can help the primary antibiotic (like Penicillin) break through the bacterial wall more effectively.
2. Medications for Specialized Cases
-
Rifampin: This is almost exclusively added for patients with Prosthetic Valve Endocarditis (PVE). It has a unique ability to penetrate the "biofilm" or slimy protective layer that bacteria build on artificial surfaces like mechanical valves or pacemakers.
-
Daptomycin: Used as an alternative for patients who cannot tolerate Vancomycin or for infections that are resistant to standard treatments.
-
Amphotericin B or Fluconazole: These are antifungals, used only in rare cases where the infection is caused by a fungus rather than bacteria. Fungal endocarditis is more difficult to treat and often requires a combination of these drugs and surgery.
3. Clinical Monitoring and Safety
Because these medications for Endocarditis are administered at high doses for 4 to 8 weeks, safety monitoring is a core part of the treatment protocol:
-
Trough Levels: For drugs like Vancomycin, we take blood samples right before your next dose to ensure the medication stays within a "therapeutic window"—high enough to kill the germ, but low enough to avoid toxicity.
-
Renal & Hepatic Panels: Weekly blood tests are conducted to monitor kidney and liver function, as these organs work hard to process the antibiotics.
-
Ototoxicity Checks: Some medications (like Gentamicin) require monitoring for side effects like dizziness or changes in hearing.
Dr. Jose A. Giron: Advanced Care & Endocarditis Treatment in Orlando
Dr. Jose A. Giron, a leading specialist in endocarditis treatment in Orlando, is a highly respected, board-certified infectious disease expert with over 40 years of clinical experience managing complex cardiovascular infections. As a Harvard-trained physician, he brings advanced expertise in diagnosing and treating infective endocarditis, including bacterial, fungal, prosthetic valve, and culture-negative cases.
His deep clinical background allows him to accurately identify the causative pathogens through precision diagnostics and implement targeted antimicrobial therapy for optimal outcomes. Dr. Giron is widely trusted for his evidence-based approach, meticulous clinical monitoring, and commitment to delivering personalized, high-quality care for patients with both acute and complicated endocarditis.
At our Orlando facility, Dr. Jose A. Giron follows a specialized, multi-step treatment protocol to ensure complete eradication of infection and protection of heart function:
Advanced Blood Culture Protocols:
Multiple blood samples are collected over time to precisely identify the bacteria or fungi responsible. This allows for highly targeted antibiotic therapy rather than relying on broad-spectrum medications.
High-Resolution Echocardiography (TTE & TEE):
We use advanced cardiac imaging to detect vegetations, valve damage, and complications. Transesophageal echocardiography (TEE) provides detailed visualization for accurate diagnosis and treatment planning.
Targeted IV Antibiotic Therapy (OPAT Available):
Because endocarditis bacteria are deeply embedded in heart vegetations, we administer high-dose intravenous antibiotics over several weeks. Stable patients may transition to Outpatient Parenteral Antimicrobial Therapy (OPAT) for continued care at home.
In-Office Infusion & Monitoring Suite:
Our facility offers hospital-grade IV infusion therapy, ensuring safe delivery of antibiotics, fluids, and supportive medications under expert supervision.
Ongoing Clinical & Laboratory Monitoring:
Regular blood tests (CBC, CRP, ESR, kidney and liver panels) are conducted to track infection response and ensure medication safety throughout the treatment duration.
Surgical Coordination (If Required):
In severe cases involving valve destruction or abscess formation, Dr. Giron collaborates closely with cardiac surgeons for timely intervention and post-surgical infection control.
Patients across Orlando rely on Dr. Jose A. Giron for his precision-driven care, advanced treatment protocols, and dedication to achieving complete recovery while protecting long-term heart health.
It is a life-threatening infection of the heart's inner lining or valves. It is dangerous because it creates "vegetations" (clumps of bacteria) that can destroy heart tissue, cause heart failure, or break off and travel to the brain, causing a stroke.
The earliest infective endocarditis symptoms are often "flu-like," such as a persistent fever, chills, and night sweats. Because these signs are non-specific, many people mistake the infection for a common cold until it becomes more severe.
While fever is the most common of the symptoms of endocarditis, it is possible to have a "subacute" version where the fever is very low-grade or intermittent. If you have a heart condition and feel unusual fatigue or body aches, you should still seek medical advice.
People with prosthetic (artificial) heart valves, prior heart defects, or those who use intravenous drugs are at the highest risk. Additionally, anyone with a history of infective endocarditis is more likely to develop it again in the future.
Yes. Acute cases involve sudden high fever and rapid heart damage. Subacute infective endocarditis symptoms develop slowly over weeks, often presenting as mild weight loss, fatigue, and vague joint pain.
Yes. Certain dental procedures can push bacteria from the mouth into the bloodstream. If your heart valves are already damaged or artificial, these bacteria can "snag" on the valve and lead to infective endocarditis.
Two specific symptoms of endocarditis are Janeway lesions (painless red spots on palms/soles) and Osler’s nodes (painful bumps on fingers/toes). These are caused by immune reactions or tiny blood clots traveling from the heart.
No. You cannot "catch" this from someone else. It is caused by your own body's reaction to bacteria entering your bloodstream from elsewhere, such as your mouth, skin, or a medical catheter.
Diagnosis usually requires a combination of multiple blood cultures to identify the germ and an echocardiogram (an ultrasound of the heart) to look for vegetations or valve damage.
Typically, no. Because the infection is deep inside heart tissue, it usually requires high-dose intravenous (IV) antibiotics for 4 to 8 weeks. However, many patients can finish this treatment at home via a PICC line once they are stable.

